Efficacy of Topical Hydroquinone 4% with or without Intradermal Autologous Platelet-rich Plasma in Lichen Planus Pigmentosus: A Split-face Randomized Controlled Trial
DOI:
https://doi.org/10.59796/jcst.V16N2.2026.184Keywords:
hydroquinone, autologous platelet-rich plasma, lichen planus pigmentosus, split-faceAbstract
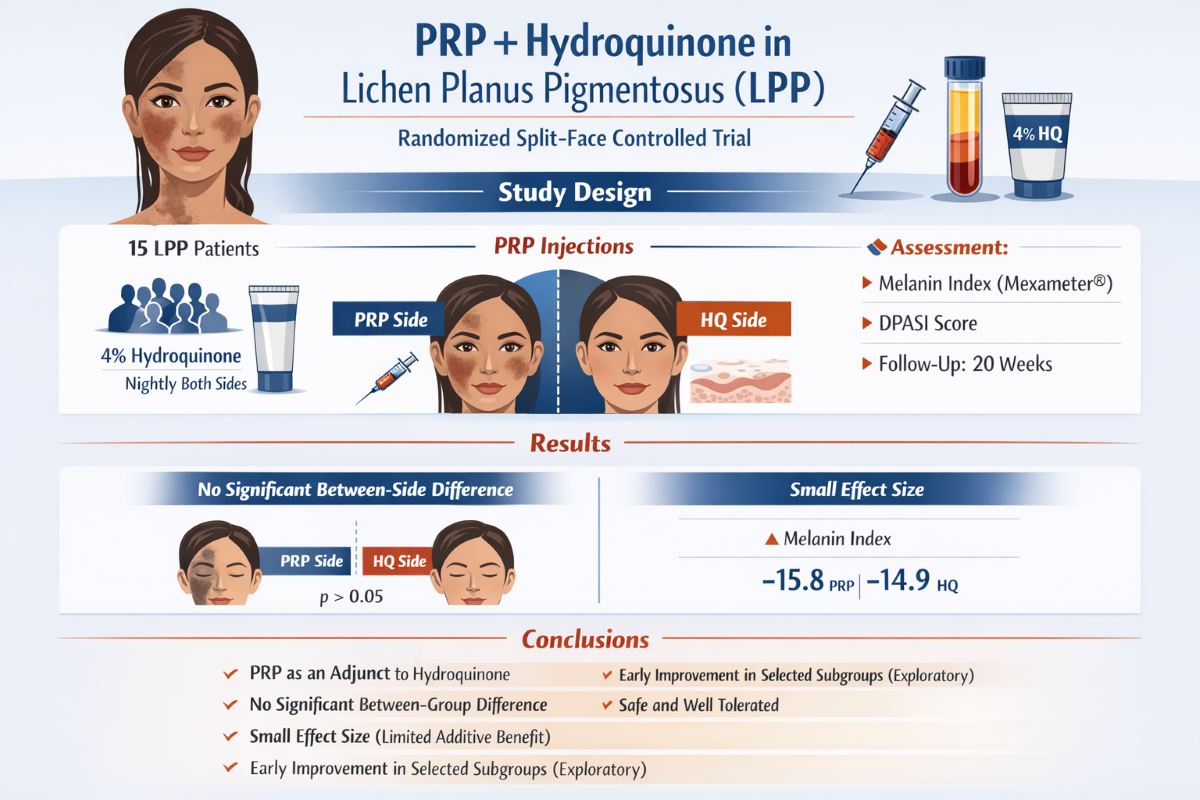
Lichen planus pigmentosus (LPP) is a chronic acquired hyperpigmentation disorder predominantly affecting sun-exposed areas of the face and neck, for which effective treatment remains challenging. Platelet-rich plasma (PRP) contains growth factors and bioactive mediators, including transforming growth factor-β1 (TGF-β1) and macromolecular activators of phagocytosis, which may modulate melanocyte activity, inflammation, and dermal pigment clearance. This study evaluated whether intradermal autologous PRP provides additive benefit when combined with topical 4% hydroquinone (HQ) in patients with LPP.
In this randomized, single-blinded, split-face controlled trial, 15 patients received intradermal PRP injections on one randomly assigned side of the face at baseline, week 2, and week 4, while both sides received nightly topical 4% HQ throughout the 20-week study period. Outcomes included the melanin index measured by Mexameter®, the hemi-modified acquired macular hyperpigmentation and severity index (DPASI), patient satisfaction, and adverse events, assessed through week 20.
Both treatment arms showed significant reductions in melanin index from baseline to week 20. Earlier reductions were observed on the PRP-treated side, particularly among patients with mild disease and those naïve to PRP. These findings are consistent with PRP-mediated modulation of melanocyte activity and inflammatory pathways. However, no statistically significant between-side differences were detected at any time point, and effect sizes were small. DPASI scores improved modestly in both groups without significant intergroup differences, while patient satisfaction favored the PRP-treated side. Adverse effects were mild and transient.
In conclusion, PRP may exert early localized biological effects on pigmentation through growth factor-mediated mechanisms but did not confer a sustained or clinically dominant advantage over HQ monotherapy. PRP appears to be best positioned as a safe adjunctive therapy in selected patients with LPP.
References
Akaranuchat, N., & Kongkunnavat, N. (2024). Improvement in the youthfulness of facial skin after a single treatment with platelet-rich plasma. Siriraj Medical Journal, 76(11), 781–788. https://doi.org/10.33192/smj.v76i11.270077
Alsousou, J., Ali, A., Willett, K., & Harrison, P. (2013). The role of platelet-rich plasma in tissue regeneration. Platelets, 24(3), 173-182. https://doi.org/10.3109/09537104.2012.684730
Bhari, N., Sharma, V. K., Singh, S., Parihar, A., & Arava, S. (2020). Effect of Q‐switched Nd‐YAG laser on the clinical, pigmentary, and immunological markers in patients with lichen planus pigmentosus: A pilot study. Dermatologic Therapy, 33(2), Article e13208. https://doi.org/10.1111/dth.13208
Bhutani, L. K., Bedi, T. R., Pandhi, R. K., & Nayak, N. C. (2009). Lichen planus pigmentosus. Dermatologica, 149(1), 43–50. https://doi.org/10.1159/000251470
Cheng, H. M., Chuah, S. Y., Gan, E. Y., Jhingan, A., & Thng, S. T. G. (2018). A retrospective clinico‐pathological study comparing lichen planus pigmentosus with ashy dermatosis. Australasian Journal of Dermatology, 59(4), 322-327. https://doi.org/10.1111/ajd.12813
Choi, M. E., Lim, Y., Lee, W. J., Won, C. H., Lee, M. W., & Chang, S. E. (2022). Characteristics of Riehl melanosis in an ethnic Asian population: A comparative study according to age, sex, and hair dye use. JEADV Clinical Practice, 1(3), 219-228. https://doi.org/10.1002/jvc2.44
Haddad, A. L., Matos, L. F., Brunstein, F., Ferreira, L. M., Silva, A., & Costa Jr, D. (2003). A clinical, prospective, randomized, double‐blind trial comparing skin whitening complex with hydroquinone vs. placebo in the treatment of melasma. International Journal of Dermatology, 42(2), 153-156. https://doi.org/10.1046/j.1365-4362.2003.01621.x
Honigman, A., & Rodrigues, M. (2023). Differential diagnosis of melasma and hyperpigmentation. Dermatological Reviews, 4(1), 30-37. https://doi.org/10.1002/der2.144
Kiatsurayanon, C., Deeudomwongsa, P., Pituvong, P., & Sajjachareonpong, P. (2025). The efficacy of platelet‐rich plasma in facial lichen planus pigmentosus: A Prospective pilot study. Health Science Reports, 8(4), Article e70455. https://doi.org/10.1002/hsr2.70455
Kim, D. S., Park, S. H., & Park, K. C. (2004). Transforming growth factor-β1 decreases melanin synthesis via delayed extracellular signal-regulated kinase activation. The International Journal of Biochemistry & Cell Biology, 36(8), 1482-1491. https://doi.org/10.1016/j.biocel.2003.10.023
Klaisung, N., Sajjachareonpong, P., Thongkaow, S., Dornphai, P., & Tienthavorn, T. (2024). Comparative effectiveness of 20% azelaic acid with 1064-Nm Nd: YAG picosecond laser vs azelaic acid alone for melasma treatment in Thai female patients: A split-face study. Journal of Current Science and Technology, 14(2), Article 41. https://doi.org/10.59796/jcst.V14N2.2024.41
Kumar, Y. H. K., & Babu, A. R. (2014). Segmental lichen planus pigmentosus: An unusual presentation. Indian Dermatology Online Journal, 5(2), 157-159. https://doi.org/10.4103/2229-5178.131087
Kumaran, M. S., Dabas, G., Vinay, K., & Parsad, D. (2019). Reliability assessment and validation of the dermal pigmentation area and severity index: a new scoring method for acquired dermal macular hyperpigmentation. Journal of the European Academy of Dermatology and Venereology, 33(7), 1386-1392. https://doi.org/10.1111/jdv.15516
Muthu, S. K., Narang, T., Saikia, U. N., Kanwar, A. J., Parsad, D., & Dogra, S. (2016). Low‐dose oral isotretinoin therapy in lichen planus pigmentosus: An open‐label non‐randomized prospective pilot study. International Journal of Dermatology, 55(9), 1048-1054. https://doi.org/10.1111/ijd.13293
Ogawa, Y., Sakamoto, H., Oryu, M., Shinnou, M., Sakamoto, N., Yanghong, W., ... & Nishioka, M. (2000). Production of macromolecular activators of phagocytosis by lysed platelets. Thrombosis Research, 97(5), 297-306. https://doi.org/10.1016/S0049-3848(99)00178-4
Sakamoto, H., Wu, B., Nagai, Y., Tanaka, S., Onodera, M., Ogawa, T., & Ueno, M. (2011). Platelet high-density lipoprotein activates transferrin-derived phagocytosis activators, MAPPs, following thrombin digestion. Platelets, 22(5), 371-379. https://doi.org/10.3109/09537104.2010.533797
Tanantong, T., Chalarak, N., Jirattisak, S., Tanantong, K., & Srijiranon, K. (2025). A study on area assessment of psoriasis lesions using image augmentation and deep learning: Addressing the lack of Thai skin disease data. Journal of Current Science and Technology, 15(3), Article 119. https://doi.org/10.59796/jcst.V15N3.2025.119
Vinay, K., Dabas, G., Parsad, D., & Kumaran, M. S. (2018). A novel scale for measurement of acquired dermal macular hyperpigmentation severity. Journal of the European Academy of Dermatology & Venereology, 32(6), e251–e253. https://doi.org/10.1111/jdv.14772
Downloads
Published
How to Cite
Issue
Section
Categories
License
Copyright (c) 2026 Journal of Current Science and Technology

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.