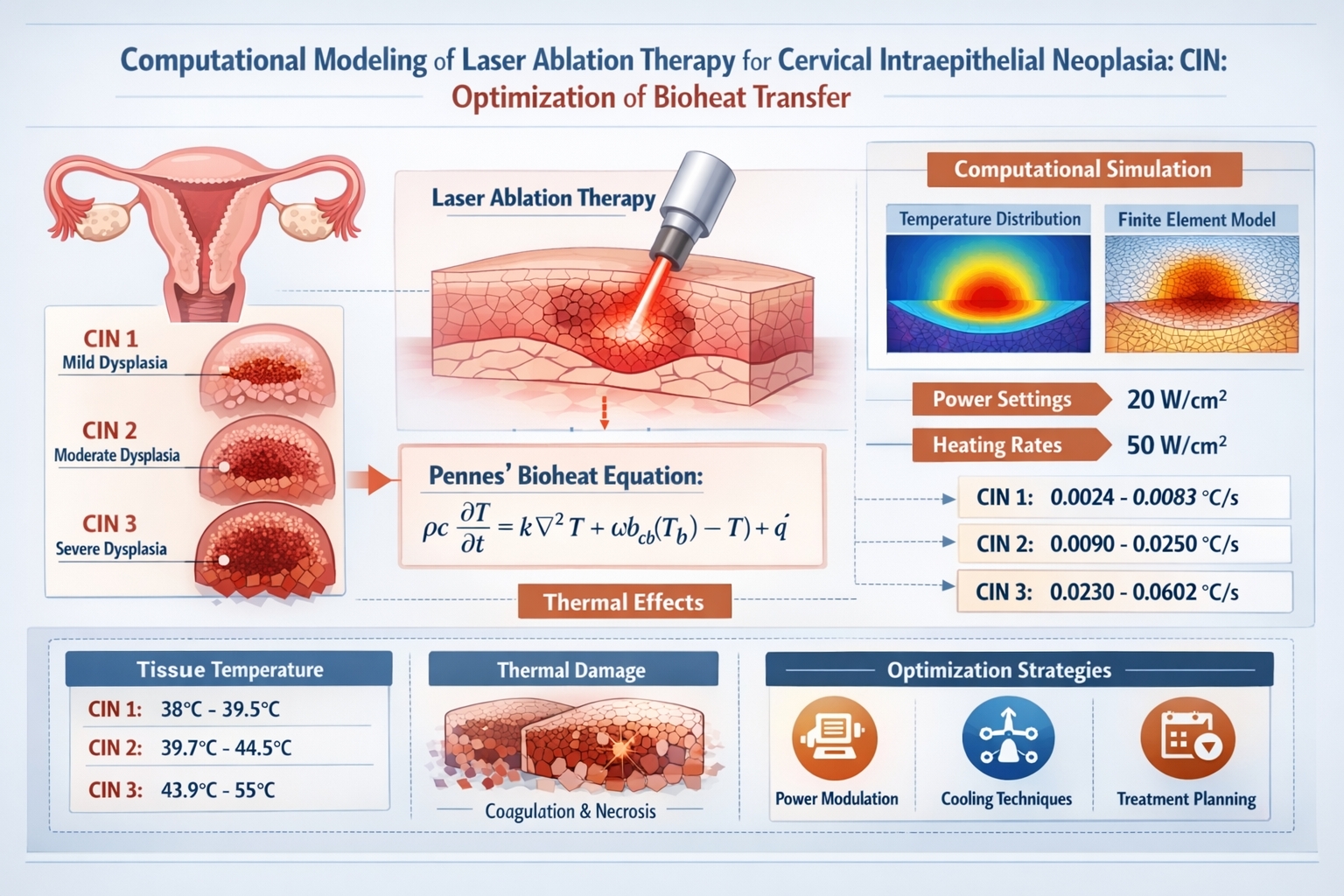
Computational Modeling of Laser Ablation Therapy for Cervical Intraepithelial Neoplasia: Optimization of Bioheat Transfer
DOI:
https://doi.org/10.59796/jcst.V16N2.2026.178Keywords:
cervical intraepithelial neoplasia, computational fluid dynamics, thermal analysis, laser ablation, Pennes’s bioheat equationAbstract
Cervical intraepithelial neoplasia (CIN) is a common precancerous condition that is treatable with laser therapy. This study presents a computational thermal analysis of CIN tissue under laser ablation, focusing on CIN1, CIN2, and CIN3 stages. Using computational fluid dynamics (CFD) and high-resolution meshing, thermal responses were evaluated under laser power settings of 20 W/cm² to 50 W/cm². Mesh complexity increased with lesion severity: CIN1 included 683 vertices and 172 triangular elements (average quality 0.9147), CIN2 had 707 vertices and 241 elements (average quality 0.9226), and CIN3 used 7,181 vertices and 14,023 elements (average quality 0.945). Thermal analysis showed that CIN1 reached 38.28 °C at 20 W/m² and 39.49 °C at 50 W/m², with heating rates of 0.0024 °C/s and 0.0083 °C/s, respectively. CIN2 peaked at 39.71 °C and 44.51 °C with heating rates of 0.0090 °C/s and 0.0250 °C/s while CIN3 reached 43.91 °C and 55.07 °C, with heating rates of 0.0230 °C/s and 0.0602 °C/s, respectively. The results indicate that higher power settings lead to more aggressive thermal gradients and faster heating, particularly in advanced CIN stages. These findings emphasize the importance of power modulation in simulating ablation outcomes.
References
Akulova, D. V., & Sheremet, M. A. (2024). Mathematical simulation of bio-heat transfer in tissues having five layers in the presence of a tumor zone. Mathematics, 12(5), Article 676. https://doi.org/10.3390/math12050676
Armstrong, G. M., & Ragupathy, K. (2022). Test of cure and beyond: Superiority of thermal ablation over LLETZ in the treatment of high-grade CIN. Archives of Gynecology and Obstetrics, 306(5), 1815-1820. https://doi.org/10.1007/s00404-022-06409-3
Athanasiou, A., Veroniki, A. A., Efthimiou, O., Kalliala, I., Naci, H., Bowden, S., ... & Kyrgiou, M. (2022). Comparative effectiveness and risk of preterm birth of local treatments for cervical intraepithelial neoplasia and stage IA1 cervical cancer: A systematic review and network meta-analysis. The Lancet Oncology, 23(8), 1097-1108. https://doi.org/10.1016/S1470-2045(22)00334-5
Azizi, M. K., & Alotaibi, A. A. (2020). Photonic jet suitable for high precision contact laser surgery applications in water. Engineering, Technology & Applied Science Research, 10(2), 5565-5569. https://doi.org/10.48084/etasr.3453
Bashkatov, A. N., Zakharov, V. P., Bucharskaya, A. B., Borisova, E. G., Khristoforova, Y. A., Genina, E. A., & Tuchin, V. V. (2020). Malignant tissue optical properties. Multimodal Optical Diagnostics of Cancer. Cham: Springer International Publishing. https://doi.org/10.1007/978-3-030-44594-2_1
Belinson, S. E., Ledford, K., Rasool, N., Rollins, A., Wilan, N., Wang, C., ... & Belinson, J. L. (2013). Cervical epithelial brightness by optical coherence tomography can determine histological grades of cervical neoplasia. Journal of Lower Genital Tract Disease, 17(2), 160-166. https://doi.org/10.1097/LGT.0b013e31825d7bf0
Boontatao, P., Pannucharoenwong, N., Sermlao, P., & Panvichien, S. (2025). Generalized dual-phase-lag modeling of rectal wall thermal protection in prostate laser therapy using hyaluronic acid, collagen, and balloon spacers. International Journal of Heat and Mass Transfer, 253, Article 127570. https://doi.org/10.1016/j.ijheatmasstransfer.2025.127570
Chimakurthi, S., Nucci, M., Blades, E., Jacques, S. L., London, R. A., & Wharmby, A. (2021, April). A computational framework for multiphysics and multiscale modeling of laser interactions with biological tissue. Bio-Optics: Design and Application. Washington, US: Optica Publishing Group. https://doi.org/10.1364/BODA.2021.DTu3A.4
Collier, T., Arifler, D., Malpica, A., Follen, M., & Richards-Kortum, R. (2003). Determination of epithelial tissue scattering coefficient using confocal microscopy. IEEE Journal of Selected Topics in Quantum Electronics, 9(2), 307-313. https://doi.org/10.1109/JSTQE.2003.814413
Donkoh, E. T., Agyemang-Yeboah, F., Asmah, R. H., & Wiredu, E. K. (2019). Prevalence of cervical cancer and pre-cancerous lesions among unscreened Women in Kumasi, Ghana. Medicine, 98(13), Article e14600. https://doi.org/10.1097/MD.0000000000014600
Frappart, L., Berger, G., Grimaud, J. A., Chevalier, M., Bremond, A., Rochet, Y., & Feroldi, J. (1982). Basement membrane of the uterine cervix: Immunofluorescence characteristics of the collagen component in normal or atypical epithelium and invasive carcinoma. Gynecologic Oncology, 13(1), 58-66. https://doi.org/10.1016/0090-8258(82)90009-9
Ghangas, S., & Kumar, R. (2025). Analysis of nonlocal bioheat transfer model with temperature dependent thermal conductivity during thermal ablation. Interactions, 246(1), Article 61. https://doi.org/10.1007/s10751-025-02280-1
Inaba, K., Nagasaka, K., Kawana, K., Arimoto, T., Matsumoto, Y., Tsuruga, T., ... & Fujii, T. (2014). High‐risk human papillomavirus correlates with recurrence after laser ablation for treatment of patients with cervical intraepithelial neoplasia 3: A long‐term follow‐up retrospective study. Journal of Obstetrics and Gynaecology Research, 40(2), 554-560. https://doi.org/10.1111/jog.12196
Inogamov, N. A., Petrov, Y. V., Khokhlov, V. A., & Zhakhovskii, V. V. (2020). Laser ablation: Physical concepts and applications. High Temperature, 58(4), 632-646. https://doi.org/10.1134/S0018151X20040045
IT’IS Foundation. (n.d.). Virtual population: High-resolution human, animal, and tissue models for biomedical applications. Retrieved from https://itis.swiss/virtual-population/
Kim, H. J., Um, S. H., Kang, Y. G., Shin, M., Jeon, H., Kim, B. M., ... & Yoon, K. (2023). Laser–tissue interaction simulation considering skin-specific data to predict photothermal damage lesions during laser irradiation. Journal of Computational Design and Engineering, 10(3), 947-958. https://doi.org/10.1093/jcde/qwad033
Kishi, Y., Hashimoto, Y., Sakamoto, Y., & Inui, S. (1987). Thickness of uninvolved fibromuscular stroma and extrauterine spread of carcinoma of the uterine cervix. Cancer, 60(9), 2331-2336. https://doi.org/10.1002/1097-0142(19871101)60:9%3C2331::AID-CNCR2820600936%3E3.0.CO;2-O
Saemathong, J., Pannucharoenwong, N., Mongko, V., Vongpradubchai, S., & Rattanadecho, P. (2023). Analyzing two laser thermal energy calculation equations: A comparison of beer-Lambert's law and light transport equation. Engineered Science, 24(2), Article 912. https://doi.org/10.30919/es912
Sajjadi, A. Y., Mitra, K., & Guo, Z. (2013). Thermal analysis and experiments of laser− tissue interactions: A review. Heat Transfer Research, 44(3-4), 345-388. https://doi.org/10.1615/HeatTransRes.2012006425
Seidabadi, L., Vandenbussche, I., Carter Fink, R., Moore, M., McCorkendale, B., & Esmailie, F. (2025). Role of computational modelling in enhancing thermal safety during cardiac ablation. Interdisciplinary CardioVascular and Thoracic Surgery, 40(8), Article ivaf184. https://doi.org/10.1093/icvts/ivaf184
Singh, S., & Melnik, R. (2020). Thermal ablation of biological tissues in disease treatment: A review of computational models and future directions. Electromagnetic Biology and Medicine, 39(2), 49-88. https://doi.org/10.1080/15368378.2020.1741383
Suzuki, W., Ietani, K., Makabe, T., Oki, S., Ohno, A., Mikami, Y., & Yamashita, H. (2024). Prognostic outcome of cervical laser ablation using a holmium yttrium-aluminum-garnet (Ho: YAG) laser for the treatment of cervical intraepithelial neoplasia: A single-center retrospective study. Gynecologic Oncology Reports, 53, Article 101405. https://doi.org/10.1016/j.gore.2024.101405
Waghe, T., Acharya, N., & Waghe Jr, T. (2024). Advancements in the management of cervical intraepithelial neoplasia: A comprehensive review. Cureus, 16(4), Article e58645. https://doi.org/10.7759/cureus.58645
Walker, D. C., Brown, B. H., Smallwood, R. H., Hose, D. R., & Jones, D. M. (2002). Modelled current distribution in cervical squamous tissue. Physiological Measurement, 23(1), 159-168. https://doi.org/10.1088/0967-3334/23/1/315
Wongchadakul, P., & Rattanadecho, P. (2021). Mathematical modeling of multilayered skin with embedded tumor through combining laser ablation and nanoparticles: Effects of laser beam area, wavelength, intensity, tumor absorption coefficient and its position. International Journal of Heat and Technology, 39(1), 89–100. https://doi.org/10.18280/ijht.390109
World Health Organization. (2019). WHO guidelines for the use of thermal ablation for cervical pre-cancer lesions. World Health Organization. Retrieved from https://apps.who.int/iris/bitstream/handle/10665/329299/9789241550598-eng.pdf
Xiao, L., Guo, J., Wang, H., He, Q., Xu, Y., Yuan, L., ... & Chen, H. (2023). Thermal damage and the prognostic evaluation of laser ablation of bone tissue a review. Lasers in Medical Science, 38(1), Article 205. https://doi.org/10.1007/s10103-023-03868-1
Xu, M., Xu, D., Deng, Z., Tian, G., & Jiang, T. A. (2023). Long-term outcomes of endoscopic ultrasound-guided laser ablation for liver tumors in the caudate lobe: 5 years of experience. Scandinavian Journal of Gastroenterology, 58(5), 558-564. https://doi.org/10.1080/00365521.2022.2148833
Downloads
Published
How to Cite
Issue
Section
Categories
License
Copyright (c) 2026 Journal of Current Science and Technology

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.